Altitude sickness is the most common medical condition affecting travelers at high elevations. In its mild form it is self-limiting and resolves after a day of rest, but if neglected it can progress within hours to high-altitude cerebral edema (HACE) or high-altitude pulmonary edema (HAPE) — life-threatening emergencies that require immediate evacuation. This complete guide explains everything you need before an expedition: how to recognize early symptoms, when to take acetazolamide, how acclimatization works, and what to do when a companion starts behaving strangely.

Altitude sickness in a nutshell
- AMS (Acute Mountain Sickness) — mild form. Headache, nausea, fatigue. Affects 25–50% of travelers above 3500 m.
- HACE — cerebral edema. Near 100% mortality untreated. Key symptom: ataxia (loss of balance).
- HAPE — pulmonary edema. Dyspnea at rest = alarm. More common than HACE.
- 300–500 m rule: above 3000 m do not raise sleeping altitude faster than 300–500 m/day.
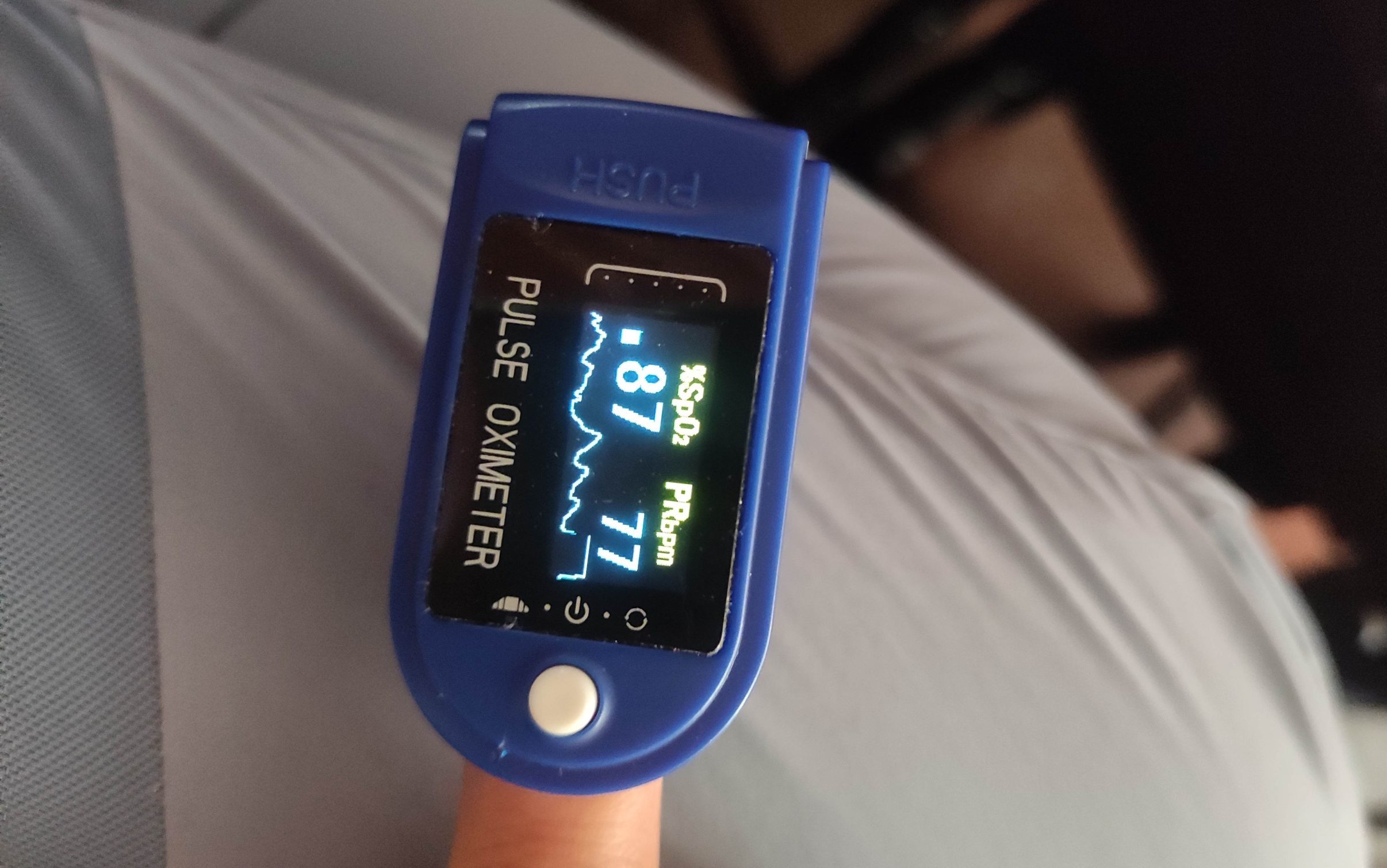
- SpO₂ 70% at 5000 m in a person who feels well is normal — treat the patient, not the number.
- The only effective treatment for severe forms — immediate descent plus oxygen.
What is altitude sickness?
The umbrella term “altitude sickness” covers three distinct entities sharing one cause — hypoxia caused by reduced atmospheric pressure at altitude:
- AMS (Acute Mountain Sickness) — the mild form. Headache plus at least one of: nausea, fatigue, dizziness. Reversible.
- HACE (High-Altitude Cerebral Edema) — life-threatening. Without treatment, death within hours.
- HAPE (High-Altitude Pulmonary Edema) — also life-threatening. More common than HACE and often appears without preceding AMS.
AMS, HACE and HAPE are not always consecutive “stages” of the same disease. HAPE can strike someone without prior AMS symptoms — especially after rapid ascent or in individuals with genetic predisposition. In expedition practice HAPE is seen roughly three times more often than HACE.
Pathophysiology — why we feel bad at altitude
Counterintuitively, on the summit of Mount Everest the percentage of oxygen in air remains identical to sea level — around 21%. What changes is atmospheric pressure. At 5364 m (Everest Base Camp) it is about 540 hPa — half the sea-level value. Oxygen molecules are more dispersed and fewer reach the alveoli with each breath.
The body responds with compensatory changes: respiratory rate rises, cardiac output increases, kidneys excrete bicarbonate, and bone marrow produces more red cells. When these mechanisms cannot keep up — hypoxic tissue damage appears, capillary leakage in lungs (HAPE) or brain (HACE), and classic AMS symptoms. Worth knowing: if Mount Everest were located in Alaska, climbing it without supplemental oxygen would be physiologically impossible — because of even lower atmospheric pressure far from the equator.
At what altitude does altitude sickness start?
- 1500–2500 m — in especially susceptible people (after illness, dehydrated) headaches and fatigue possible.
- 2500–3500 m — first AMS symptoms in approximately 20% of travelers, especially after rapid car or cable-car ascent.
- 3500–5000 m — AMS affects 25–50% of population; first HAPE and HACE cases.
- 5000–6000 m — threshold of severe symptoms. Clinical observation during expedition medical care in the Everest region: first serious problems between 4000 and 5000 m, but the real line above which it is hard to find anyone symptom-free is around 5000 m.
- Above 6000 m — deterioration processes begin to outweigh regeneration. Extended stays become exhausting.
- Above 8000 m (“death zone”) — acclimatization is impossible. Every minute without oxygen brings the body closer to death.

Risk factors: previous AMS/HAPE/HACE episode, rapid ascent (less than 300 m/day above 3000 m), dehydration, respiratory infection, alcohol consumption, certain medications (e.g. strong sedatives).
AMS symptoms and Lake Louise Score
The main and earliest AMS symptom is headache — it may affect up to 70% of trekkers above 3500 m. Other classic symptoms:
- Loss of appetite, nausea, vomiting
- Fatigue and weakness out of proportion to effort
- Dizziness
- Sleep disturbances (insomnia, Cheyne-Stokes breathing)
The Lake Louise Score — a standardized tool developed by mountain medicine physicians — is used to grade severity. Each of four symptoms scores 0–3 and the sum falls into one of three brackets:
| Symptom | Severity | Points |
|---|---|---|
| Headache | none / mild / moderate / disabling | 0 / 1 / 2 / 3 |
| GI symptoms | none / poor appetite / moderate nausea / severe vomiting | 0 / 1 / 2 / 3 |
| Fatigue/weakness | none / mild / moderate / disabling | 0 / 1 / 2 / 3 |
| Dizziness | none / mild / moderate / disabling | 0 / 1 / 2 / 3 |
3–5 points: mild AMS
Rest, hydration (2–4 L/day with electrolytes), analgesics (500–1000 mg paracetamol every 6 h, 200–400 mg ibuprofen, 500–1000 mg metamizole). Do not ascend until symptoms resolve. Most cases resolve within 24–48 h at the same altitude.
6–9 points: moderate AMS
The person may stay at current altitude but absolutely must not ascend. Management as for mild AMS + consider acetazolamide 125–250 mg twice daily. If symptoms do not resolve within 24 h or SpO₂ drops significantly — descend 500–1000 m.
10–12 points: severe AMS
Condition immediately preceding or already life-threatening. HACE or HAPE can develop any moment. Give acetazolamide 250 mg twice daily and initiate evacuation: 500–1000 m descent on foot (stabilizing position, with escort) or by helicopter, depending on patient condition and terrain.
High-altitude cerebral edema (HACE)
HACE is brain tissue swelling caused by hypoxia and capillary leakage. Tissue compressed by the skull causes neurological disturbances — balance centers rupture first (located in the posterior cranial fossa, particularly susceptible to pressure).
Key HACE symptoms
- Ataxia (loss of balance) — patient cannot walk a straight line, cannot stand stable with eyes closed
- Agitation or confusion — slurred speech, illogical responses
- Severe headache unresponsive to painkillers
- SpO₂ often <50% — critically low
- Vomiting, sometimes papilledema
A characteristic case from expedition practice: a participant reports weakness and diarrhea in the evening; the team assumes food poisoning. During the night he collapses in the lodge corridor — slurred speech, agitation, unable to stand. SpO₂ 50%. Diagnosis: HACE. Management: oxygen + dexamethasone + helicopter evacuation at dawn. The patient survives because action was taken within hours, not days.
More on diagnosis and treatment in a dedicated article — HACE — recognition and treatment.
High-altitude pulmonary edema (HAPE)
HAPE is fluid leakage from pulmonary capillaries into alveoli. Mechanism: hypoxia causes pulmonary vasoconstriction → pressure rises → microvascular damage → fluid in alveolar space → impaired gas exchange. The patient literally “drowns in their own fluids”.
Key HAPE symptoms
- Dyspnea at rest — this is the alarm signal. Exertional breathlessness at altitude is normal; dyspnea while sitting or standing = HAPE until proven otherwise.
- Persistent cough, often with pink or bloody sputum (foamy exudate)
- Chest tightness, feeling of “lung congestion”
- Rapid breathing and elevated heart rate
- Audible crackles on auscultation, sometimes even without stethoscope
More on diagnosis and treatment — HAPE — recognition and treatment.
Differential diagnosis — is it really AMS?
Not every headache at altitude is AMS. Worth excluding common “mimickers”:
| Problem | Key differentiator |
|---|---|
| Dehydration | dark urine, dry mucous membranes; symptoms resolve after 1 L electrolytes within 1–2 h |
| Cold / sinus infection | runny nose, sinus pain, fever; response to standard analgesics “as at sea level” |
| Migraine | pulsatile unilateral, aura, photophobia, migraine history |
| Physical exhaustion | resolves after 2–4 h rest, no other AMS features |
| Hypoglycemia | headache + tremor + sweating; resolves after carbs |
| CO poisoning (tent!) | headache + nausea + drowsiness after time in closed tent with stove |
Practical rule: if symptoms resolve after 24 h rest at the same altitude + hydration + paracetamol — likely mild AMS or combined dehydration/exhaustion. If they worsen or ataxia or resting dyspnea develops — assume HACE/HAPE and initiate descent.
When to descend — the golden rules
- Descent is not failure — it is treatment. The only truly effective treatment for HACE and HAPE.
- Do not ascend with any AMS symptoms. ICAR/UIAA rule: “don’t ascend with symptoms”.
- Descend 500–1000 m for worsening moderate AMS, immediately for suspected HACE/HAPE.
- Climb high, sleep low — acclimatization touch may go higher, but sleep lower.
- The 300–500 m rule — above 3000 m do not increase sleeping altitude faster. After every 1000 m climbed — rest day.
- Never leave a sick person alone. Someone with AMS can progress to HACE within hours and be unable to call for help.
Pharmacological prophylaxis — when it makes sense
In my opinion the best and healthiest approach to acclimatization is natural acclimatization without prophylactic medication. Drugs are often overused — part of the climbing community takes acetazolamide like candy, because “everyone does”. Not everyone should.
Pharmacological prophylaxis is worth considering when:
- Previous episode of severe AMS, HACE or HAPE (unless we can identify a specific acclimatization error then)
- Forced rapid ascent (>500 m sleeping/day above 3000 m) due to logistics
- Expedition to regions without evacuation options (rare today, occasional on remote 6000-ers)
Most frequently used drugs in AMS prophylaxis and treatment:
- Acetazolamide (Diamox / Diuramid) — first-line drug. Prophylactic dose 125 mg twice daily, therapeutic 250 mg twice daily. Start 24 h before reaching new altitude. Details: Diamox — prophylactic and therapeutic dosing.
- Dexamethasone — first-line in HACE treatment (8 mg single dose, then 4 mg every 6 h), rarely in prophylaxis.
- Nifedipine / nitrendipine — in HAPE treatment (20–30 mg every 8 h). Not classic AMS prophylaxis.
- Ibuprofen — 600 mg three times daily has documented RCT prevention effect for AMS, weaker than acetazolamide. Alternative for sulfonamide-intolerant patients.
Acclimatization — how to do it properly
Acclimatization is a series of physiological changes enabling tolerance of lower oxygen availability. Key processes: increased minute ventilation, rising red cell count, improved muscle perfusion, mitochondrial density. Full acclimatization to a given altitude takes 2–4 weeks and persists up to 6 weeks after return to lowlands — every subsequent expedition requires fresh acclimatization.
Practical acclimatization rules
- Slow ascent: maximum 300–500 m sleeping altitude/day above 3000 m.
- Rest day after every 1000 m gained: sleep at the same altitude, day walk higher for acclimatization touch (“climb high, sleep low”).
- Hydration 3–6 L/day. Monitor urine — clear or straw = OK, darker = add electrolytes and drink more.
- Avoid alcohol during acclimatization — it depresses the respiratory center and deepens nocturnal hypoxia.
- Avoid strong sedatives — same reason.
- Monitor symptoms daily — pulse oximetry morning and evening + Lake Louise Score.
Pre-acclimatization in hypoxic tents
Some people sleep or train in hypoxic tents as preparation. Meta-analyses show some effect — particularly with sleeping at simulated altitudes of 2000–2500 m for 2–4 weeks, minimum 14 h/day. Logistically expensive but worth considering before fast expeditions (e.g. weekend Mont Blanc, time-limited Aconcagua).
Honestly — this is a tool I would use in preparation for extreme-altitude expeditions. Limitation: hypoxic tents do not fully reproduce mountain conditions as they manipulate oxygen concentration, not atmospheric pressure. Oxygen molecules are not “dispersed” as in reality.
High-risk groups
- Previous AMS/HACE/HAPE episode — re-entry HAPE risk on every subsequent expedition.
- Children — higher risk of rapid HAPE development. Most pediatric organizations advise against treks above 3500 m in children <10–12 years.
- Cardiac and pulmonary disease — uncontrolled heart failure, severe COPD, pulmonary hypertension are contraindications to expeditions above 3500 m.
- Anemia — Hb <11 g/dL in women, <12 g/dL in men — reduced oxygen transport capacity.
- Diabetes — glycemic control is harder at altitude (absorption changes, altered energy demand).
- Pregnancy — no clear guidelines, most physicians advise against trekking above 3000–3500 m due to potential fetal hypoxia effects.
Each of these situations requires individual consultation with an expedition medicine physician — not a “family doctor who writes a certificate”. The expedition plan should consider specific route, pace, evacuation options, and pharmacological reserves.
High-altitude first aid kit essentials
Minimum kit for altitude illness (beyond the general first aid kit — see complete expedition medical kit guide):
- Pulse oximeter + spare batteries (laminated card with SpO₂ norms at various altitudes)
- Acetazolamide (Diuramid) 250 mg — at least 20 tablets for a 2–3 week expedition
- Dexamethasone — tablets + pre-drawn IM injection (lateral thigh) — HACE rescue kit
- Nifedipine 20 mg (sustained-release) — HAPE rescue kit
- Paracetamol / ibuprofen / metamizole for headache
- Rescue oxygen cylinder (on larger expeditions) or base camp access
- Laminated Lake Louise Score — works without batteries
Note: acetazolamide, dexamethasone and nifedipine are prescription-only drugs. Before the expedition, meet with an expedition or travel medicine physician — a good rescue plan is one you know, with drugs on hand that you can administer.
Altitude sickness myths
“I’m fit, I won’t get sick”
Aerobic fitness does not translate to altitude sickness immunity. We see athlete-machines who push summit ascents at high pace and exactly for this reason fall ill faster — the stressed body acclimatizes worse. Humility toward altitude applies to everyone regardless of VO₂max.
“If I go slowly, there will be no problem”
Slow walking pace during the day ≠ slow acclimatization. What counts is sleeping altitude, not trail pace. You can crawl for 10 h and still exceed 500 m/night rule — result: AMS in the evening.
“Acetazolamide masks symptoms — it’s dangerous”
A myth common in Eastern European climbing circles. Acetazolamide does not “mask” symptoms — it genuinely accelerates acclimatization (increases minute ventilation via metabolic acidosis). RCT meta-analyses show reduced AMS and HAPE frequency with prophylaxis in at-risk individuals. Not a miracle, but a tool with documented efficacy.
“Sherpas are AMS-immune because they are strong”
Sherpas are adapted, not acclimatized. Adaptation is multi-generational genetic change (increased NO production, higher SpO₂ at given altitude, more efficient mitochondria). We, lowland dwellers, can achieve only acclimatization — a short-term process. You cannot “become a Sherpa” in 3 weeks.
Frequently asked questions
At what altitude does altitude sickness start?
First AMS symptoms may appear from 2000–2500 m in susceptible individuals, but statistically significant incidence (20–50%) starts at 3500 m. Above 5000 m it is hard to find someone without any symptoms — headache and poorer sleep at this altitude are normal. HACE and HAPE most often develop above 3500–4000 m.
Does Diamox really work prophylactically?
Yes. RCT meta-analyses show significant reduction in AMS incidence (30–50%) with 125 mg twice daily started 24 h before altitude exposure. Mechanism: carbonic anhydrase inhibition → metabolic acidosis → compensatory hyperventilation → better oxygen delivery. This is not marketing — it is documented pharmacology. Dosing details: /en/diamox-acetazolamide-dosing/.
How fast must descent happen in HAPE or HACE?
Immediately. In HACE every hour of delay increases mortality risk — the brain is losing oxygen. In HAPE the patient literally drowns in their own fluids. Target: at least 500–1000 m lower. Helicopter evacuation preferred; if impossible, on foot with escort (in HAPE seated position, in HACE supine with head elevated). Drugs (dexamethasone, nifedipine, oxygen) buy time — they do not replace descent.
Does hypoxic training prevent AMS?
Partially. Meta-analyses show effect with hypoxic tent sleep at simulated 2000–2500 m for minimum 14 h/day over 2–4 weeks before expedition. Short intermittent exposures (type “one-hour chamber session”) have weak or no protective effect against real-altitude AMS. Treat pre-acclimatization as an adjunct, not a substitute for gradual ascent.
How does AMS differ from HAPE and HACE?
AMS is the mild form — headache + nausea + fatigue. Reversible, not directly life-threatening. HACE is cerebral edema — the key symptom is ataxia (loss of balance) and confusion, SpO₂ often <50%. HAPE is pulmonary edema — dyspnea at rest, cough with bloody/pink sputum. HACE and HAPE are life-threatening emergencies requiring immediate evacuation; AMS only requires rest at the same altitude and possibly medication.
References
- Luks AM, Auerbach PS, Freer L, et al. Wilderness Medical Society Clinical Practice Guidelines for the Prevention and Treatment of Acute Altitude Illness: 2019 Update. Wilderness Environ Med. 2019;30(4S):S3–S18.
- Luks AM, Ainslie PN, Lawley JS, Roach RC, Simonson TS. Ward, Milledge and West’s High Altitude Medicine and Physiology, 6th ed. CRC Press, 2021.
- Hackett PH, Roach RC. High-altitude illness. N Engl J Med. 2001;345(2):107–114.
- Hidalgo R et al. High Altitude Medicine: A Case-Based Approach. Springer, 2023.
- Bärtsch P, Swenson ER. Acute high-altitude illnesses. N Engl J Med. 2013;368(24):2294–2302.
Disclaimer: This article is for informational purposes only and does not replace individual medical consultation. In life-threatening situations on expedition, call 112, TOPR 601 100 300, GOPR 985 (Poland) or your local mountain rescue.